It’s an honor to introduce you to Lisa who’s sharing her unique journey through motherhood as part of our month-long guest post series, Special Mamas. Lisa is a mom to three boys. Her oldest son, Micah, was born with a rare metabolic disorder. As you can imagine, it’s incredibly challenging to communicate a life-changing medical diagnosis in one short blog post. So today, Lisa’s journeying back to Micah’s infancy, recalling the earliest of days when he nearly lost his life. Lisa met the challenge with an incredibly intimate, honest and hopeful post. Soak it all in and send Lisa a special word of encouragement for her unique journey through motherhood.
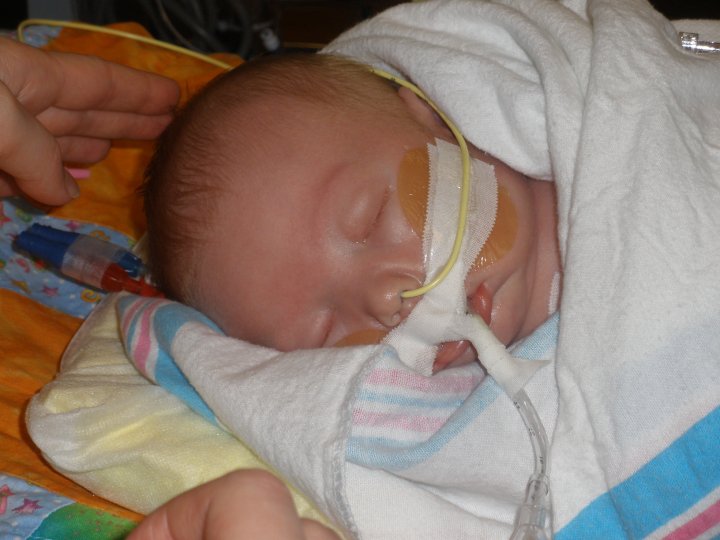
My husband almost shouted at the lady behind the glass window. She stared back, deadfaced, then chomped her gum. “It will be at least thirty minutes.”
It was the third time we had received that same answer. Somewhere behind that door to the right was our six-day-old son who had just arrived by helicopter. I’ve always heard that giving birth is the hardest thing I’ll ever do. I believed it until I stood outside the ER and watched him being put onto that helicopter. Watched it take off without me.
Sometime later a solemn nurse led us back to his room. There were tubes and wires everywhere around his bed. A doctor, with an accent almost unintelligible, mumbled facts about a condition we had never heard of and we weren’t sure he had either. He handed us a stack of papers and left; we never saw him again. That same solemn nurse told us, fumbling for words, that Micah wasn’t doing well. I wanted to scream at her, Tell me something I don’t know. Can’t you do anything?
I sat in the rocking chair and stared at his bed. There was no offer to help us hold him and what little I knew of motherhood seemed ripped away by this unexpected day. It wasn’t a family-friendly hospital: we couldn’t just stay in his room and breathe the same air as our baby. They closed down the unit when they did surgeries or brought new children in and parents had to leave.
I could walk you to where I was sitting in the waiting room when my parents arrived. They had left work as soon as Justin called them and driven the four hours to the hospital. My dad hugged me and we sat and waited while Justin went for some food. I think he needed the fresh air and space more than the chicken.
The main hallway marched through that floor of the hospital and intersected with a perpendicular section where one side led to the doors of the NICU and the other side had parent rooms and a bathroom. While I stood in that dull hallway trying to resign myself to my baby dying, a family with a little girl pushed a new mom in a wheelchair through the main hallway in front of me. I had already figured out that you didn’t want to ask about anyone else’s story; you didn’t have enough emotional energy to carry that too.
I pretended to sleep that night in a tiny, uncomfortable bed. Some stuff, most of which I didn’t need, was spilling out of a suitcase in the corner. We had gone home and packed a suitcase before we had followed the helicopter up the interstate. We had touched all the baby things in our apartment wondering if we would still need them. We even debated making a Facebook post to notify friends and family. We didn’t because we realized we didn’t know what to say. In that crowded room with faded carpet I relived the day’s events and tried to surrender my baby to God. The night dragged on but the sun finally rose and I could see out the window, across a roof, and into the pharmacy where employees were changing shifts.
That morning was a lot like the previous afternoon except they had intubated Micah during the night. One more tube snaked its way into my little boy’s body in an effort to keep him alive. Around lunchtime I sat in a booth at Fazoli’s and stared across the parking lot at a maze of flowers that decorated the front of a nursery. It was beautiful, full of life and spring, and I felt like I was dying inside. My food sat untouched except for a few bites that I ate to appease Justin.
After we visited Micah for a while I was standing in the back hallway of the NICU when a door opened and I realized that same mama with the little girl was holding her new baby while the little girl danced around. They had unplugged the baby to let the mom hold him while he died. I cried for her, my heart splintering, while I wondered if that was in my future.
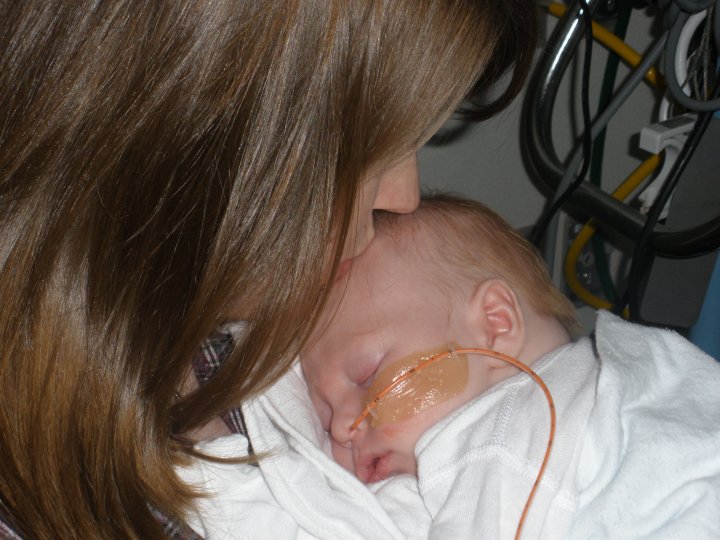
A new resident came on shift and asked us to sign paperwork for a transfer to another children’s hospital. “There’s nothing we can do here except wait and see what happens. It won’t be good.” We signed the paperwork and sat with our pastor and his wife while they made the arrangements. When I stepped out for some water Justin told them how small the chances were that Micah was going to live. A nurse came and told us we could go see Micah before they prepared him for transport. The unit was closed because of a surgery but his chance of survival was so small they took us in the back way to see him one more time.
I stood and stared at my baby in that bed. Tubes covered him; he was so puffy from fluids that he didn’t even look like the child I given birth to less than a week earlier. I sobbed into my husband’s chest and realized I wasn’t the only one crying. The resident who had arranged for the transport stood in the corner of the room with tears running down her face.
As they prepped him for the move and started transport we walked through the parking garage for the last time. They listed him as ‘unstable and nonresponsive’ and we strapped on our seat belts. That morning we had paid for a week’s worth of parking not knowing we would be leaving four hours later. We drove down the interstate. Somewhere in front of us our child was surrounded by strangers and dying.
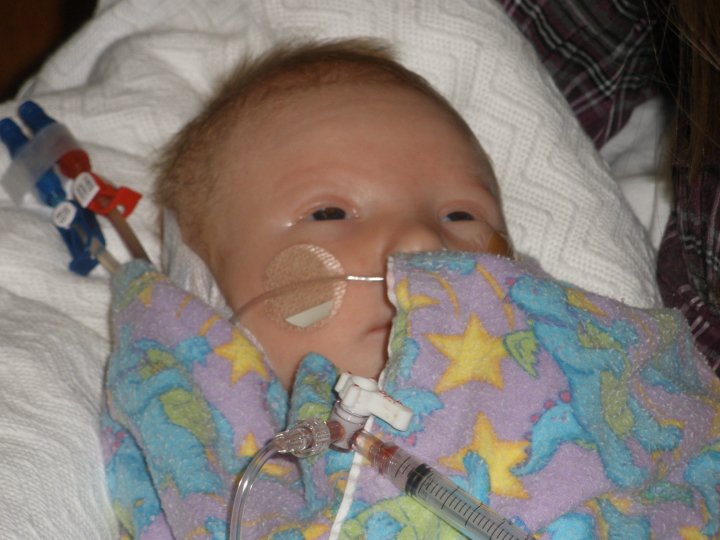
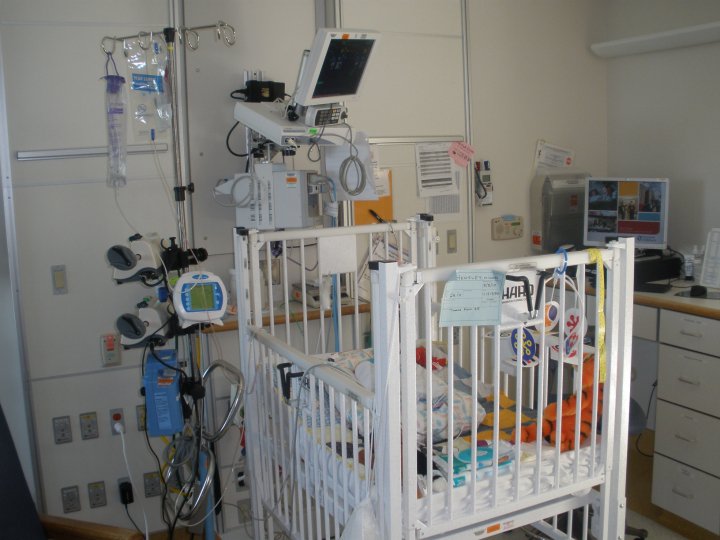
Micah has Isovaleric Acidemia, a rare metabolic disorder which causes the body to be unable to break down the essential amino acid leucine. Thanks to the work of the talented staff at Cincinnati Children’s Hospital he did survive his metabolic crisis. We spent an agonizing month in the hospital with him as they performed a risky dialysis procedure to remove toxins from his bloodstreams and then allow his body to adjust to taking in food on a controlled diet again.
Anyone who has been in the NICU knows it’s a rollercoaster of emotions, a seesaw of good news and bad news. Right before we were scheduled to be released he developed pyloric stenosis and we stayed another two weeks for diagnosis and surgery when they also placed a g-tube. (A g-tube is a feeding line that is inserted directly into the stomach through the abdomen.) It was originally intended only for emergencies but he refused to drink his medical formula until he was over a year old and I fed him through his g-tube most of the time. It was a blessing and a nightmare.

We visited the ER several times a year because of g-tube complications until he was almost five and it was taken out. It came out frequently and if we found it immediately we could replace it ourselves but a g-tube tract closes quickly and we needed medical assistance if it had been out for more than an hour. More than once, we have stood in the ER and explained to a doctor how to insert a new g-tube. We actually had one doctor refuse to replace it because he had no experience with pediatric g-tubes.
Because Isovaleric Acidemia is so rare, we know more about it than any doctors we see besides metabolic specialists. We have learned to advocate for Micah’s care because his disease is so hidden. Twice this year he has been hospitalized for complications of contracting a stomach bug. Our local hospital has been amazing dealing with us but we have had to explain the urgency of getting him treatment, which can be difficult when you arrive at the ER with a five-year-old who has thrown up three times. However a phone call from a specialist at a children’s hospital helps. Thankfully the same physician’s assistant has seen him almost every time we’ve been to the ER so we haven’t had to start at square one very often.



Micah turned six in April 2016 and one of the biggest challenges we have faced in dealing with Micah’s IVA has been not making it his “thing” yet taking it seriously. I don’t want him to use IVA as his excuse or see it as his defining characteristic. He drinks a medical formula and eats a low-protein diet as treatment of his IVA (because the amino acid leucine poisons his body in large amounts). While I count his protein now we will be starting to teach him how to manage his own diet. There are a lot of things he can’t eat – meat, dairy, and other high-protein foods – but he loves the foods he can have.
God has blessed our family with amazing people to help us care for Micah. About a year ago, my husband looked up that resident who arranged to have Micah transferred to Cincinnati Children’s and called her to thank her. She remembered Micah and said she often wondered what happened. She was thrilled to hear he was doing so well.
 Lisa Hensley is a writer and podcaster who dabbles in other creative pursuits. She and her husband have three boys and live in small-town Kentucky. Her online space encourages women to know Christ and embrace their work. You can find her at her blog www.lisahensley.me/blog/, on Instagram at instagram.com/delighting_days, Twitter at twitter.com/delighting_days, and Facebook at facebook.com/delightingdays.
Lisa Hensley is a writer and podcaster who dabbles in other creative pursuits. She and her husband have three boys and live in small-town Kentucky. Her online space encourages women to know Christ and embrace their work. You can find her at her blog www.lisahensley.me/blog/, on Instagram at instagram.com/delighting_days, Twitter at twitter.com/delighting_days, and Facebook at facebook.com/delightingdays.

This post is part of a month-long guest post series titled Special Mamas. The series runs all May and is in honor of moms who have unique journeys to and through motherhood. To read all 10 posts in the Special Mamas series, CLICK HERE and you’ll be directed to the introductory post. There, you’ll find all guest posts listed and linked for easy reading!
[…] the babies for us. I always hesitate to compare Micah’s arrival to anyone having a baby. He almost died and spent a month in the NICU, receiving a rare disease diagnosis. That’s not your average […]
[…] applause for making it through a day of children throwing up. Just a big pile of laundry and maybe a hospital visit for us. But God has gifted me with these children; it’s an honor to do whatever God has […]
Thank you for sharing your family’s journey thus far, Lisa. Praise God for Micah and for God’s faithfulness in his life. Blessings to all of you.